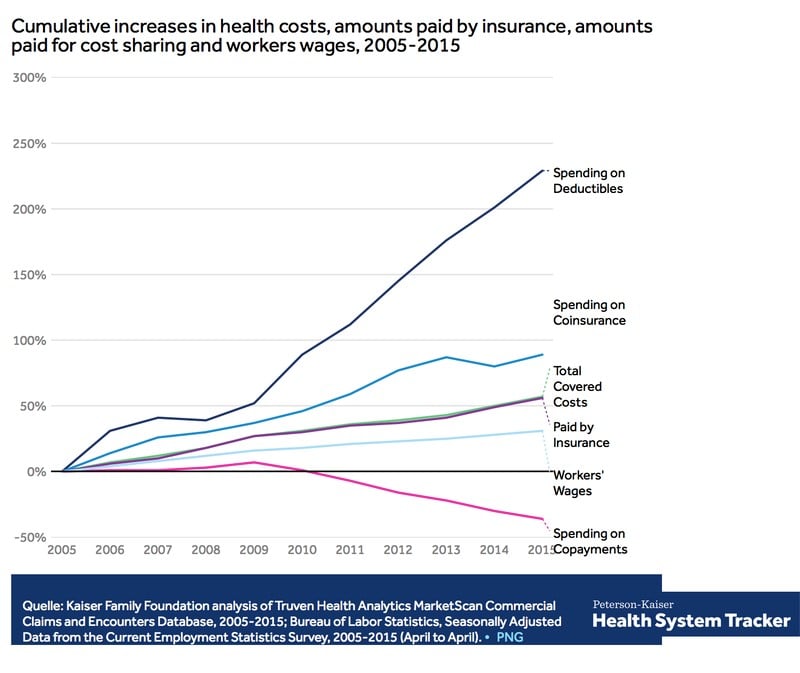
 employee health plan deductible
employee health plan deductible DPC to the rescue
direct primary care Referenced-based pricingSuzy K. Johnson, MBA, CEBS, RHU, CLTC is president, owner and employee benefit specialist at Employee Benefit Advisors of the Carolinas, LLC.
© Touchpoint Markets, All Rights Reserved. Request academic re-use from www.copyright.com. All other uses, submit a request to [email protected]. For more inforrmation visit Asset & Logo Licensing.






